Effect of Hybrid Closed-Loop Insulin Delivery on Glucose Counterregulation in Long Standing Type 1 Diabetes: A Proof of Concept, Mechanistic, Single-Arm Clinical Trial
Brief description of study
Can a type 1 diabetic adult avoid low glucoses & regain hypoglycemia awareness using a hybrid closed loop insulin delivery system?
Involvement is 22 months (13 visits) & includes a4-week Screening Phase & an 18-month Intervention Phase. 3 Hyperinsulinemic Clamps done at: Baseline (before starting to use the device & after completing the screening), 6 months (after using the device 6 months), & after using the device 18 months, will allow us to measure improvement in hypoglycemia awareness.
Detailed description of study
The purpose of this small, proof-of-concept, mechanistic study is to determine whether hybrid closed-loop insulin delivery can achieve sufficient hypoglycemia avoidance in patients with long standing type 1 diabetes experiencing hypoglycemia and symptom unawareness despite receiving intensive insulin therapy standard-of-care to improve glucose counterregulation against insulin-induced hypoglycemia. As it remains critically important to understand the potential physiologic benefits of hypoglycemia avoidance by means of a hybrid closed-loop system in this population, studying each well characterized subject as his/her own control by a within subject design should serve the study purpose, and has been the standard approach to assessing the effects of various approaches to hypoglycemia avoidance in patients with unawareness. The data generated will be available to power future randomized clinical trials to determine the comparative efficacy of emerging artificial pancreas and β-cell replacement approaches to achieve target glycemic control with amelioration of problematic hypoglycemia in type 1 diabetes.
Screening Phase At the screening visit, the study details and procedures will be discussed with a research coordinator and at least one of the PI or the research nurse practitioner. The potential participant is given adequate time to ask questions and review the informed consent document. Once satisfied that all questions have been answered, the potential participant will either decline to participate or sign the informed consent document. This may occur at a subsequent visit if the potential participant desires, in order to think further about what participation means and/or to consult with family, friends and/or a personal physician. The consent form is signed in the presence of a witness (research coordinator +/- family member). All participants must read, sign, and date a consent form before entering the study, undergoing physical examination or undergoing any testing. The informed consent form will be revised whenever important new safety information is available, whenever the protocol is amended, and/or whenever any new information becomes available that may affect participation in the studies.Eligibility will be confirmed through the performance of a history and physical examination by the PI or the research nurse practitioner, EKG, urine pregnancy test (if applicable), serum chemistries, TSH, cell counts, HbA1c and C-peptide, completion of glycemic lability and hypoglycemia awareness and hypoglycemia severity questionnaires, placement of a 7 day blinded CGM (iPro 2, Medtronic Diabetes, Northridge, CA) unless on CGM available for downloading, and 7 day accelerometry (WGT3X-BT, Actigraph LLC,) to define the nocturnal period.
Only after all eligibility criteria (inclusion and exclusion) are met, will a potential subject be enrolled. Repeated clinical testing throughout the study will ensure the continued safety and minimization of risk for the enrolled participants.
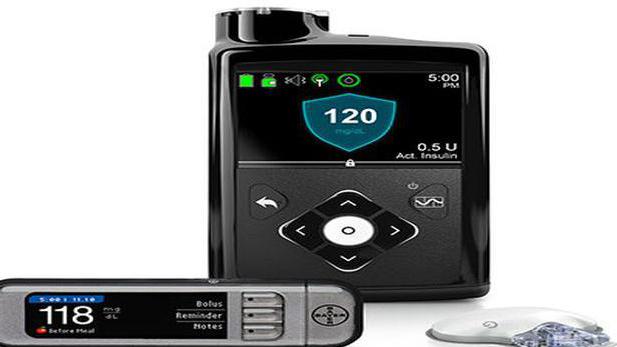
Study Intervention Phase Eligible subjects will complete a baseline assessment of glucose counterregulation by stepped- hyperinsulinemic hypoglycemic clamp prior to starting intervention with the hybrid closed-loop system (MiniMed 670G system, Medtronic Diabetes, Northridge, CA). Unless this system becomes available to the subject via their insurance carrier, one will be provided for them. Subjects will also receive a study glucometer (Contour Next Link 2.4, Bayer, Indianapolis, IN) that communicates with the MiniMed 670G insulin pump for bolus dosing calculation and glucose sensor calibration. Subjects who cannot maintain > 80% (or 6/7 day) compliance with the sensor component as assessed at each study visit may be dropped since less compliance has not been associated with any benefit of CGM to glycemic control and limits the potential for benefit from LGS on hypoglycemia avoidance. Accuracy of the sensor will be assessed at each visit through devise download and interpretation. Study visits will occur weekly for the first month, then monthly until month 6, and then every 3 months until month 18. This schedule will allow for determination of possible benefit from hybrid closed- loop insulin delivery on glucose counterregulation after 6 months of intensive provider support, and then for assessment of the durability or potential further gains in beneficial effects after another 12 months of more typical provider interaction occurring every 3 months. Weekly visits may be performed via telephone with uploading devise data to Care Link for review and interpretation. Uploaded or downloaded insulin delivery, blood and sensor glucose monitoring, insulin dose settings and CGM calibration accuracy, alert settings, time spent in auto and manual modes, and LGS threshold and activity will be assessed at each visit, targeting > 80% CGM and LGS compliance, adjusting basal and bolus insulin dosing in order to minimize glycemic excursions while maximizing hypoglycemia (
Eligibility of study
You may be eligible for this study if you meet the following criteria:
-
Conditions:
Diabetes,Type 1 diabetes,Diabetes,Hypoglycemia,Hypoglycemia,islet,Type 1 Diabetes Mellitus
-
Age: Between 25 Years - 70 Years
-
Gender: All
Updated on
27 Jul 2023.
Study ID: 827557